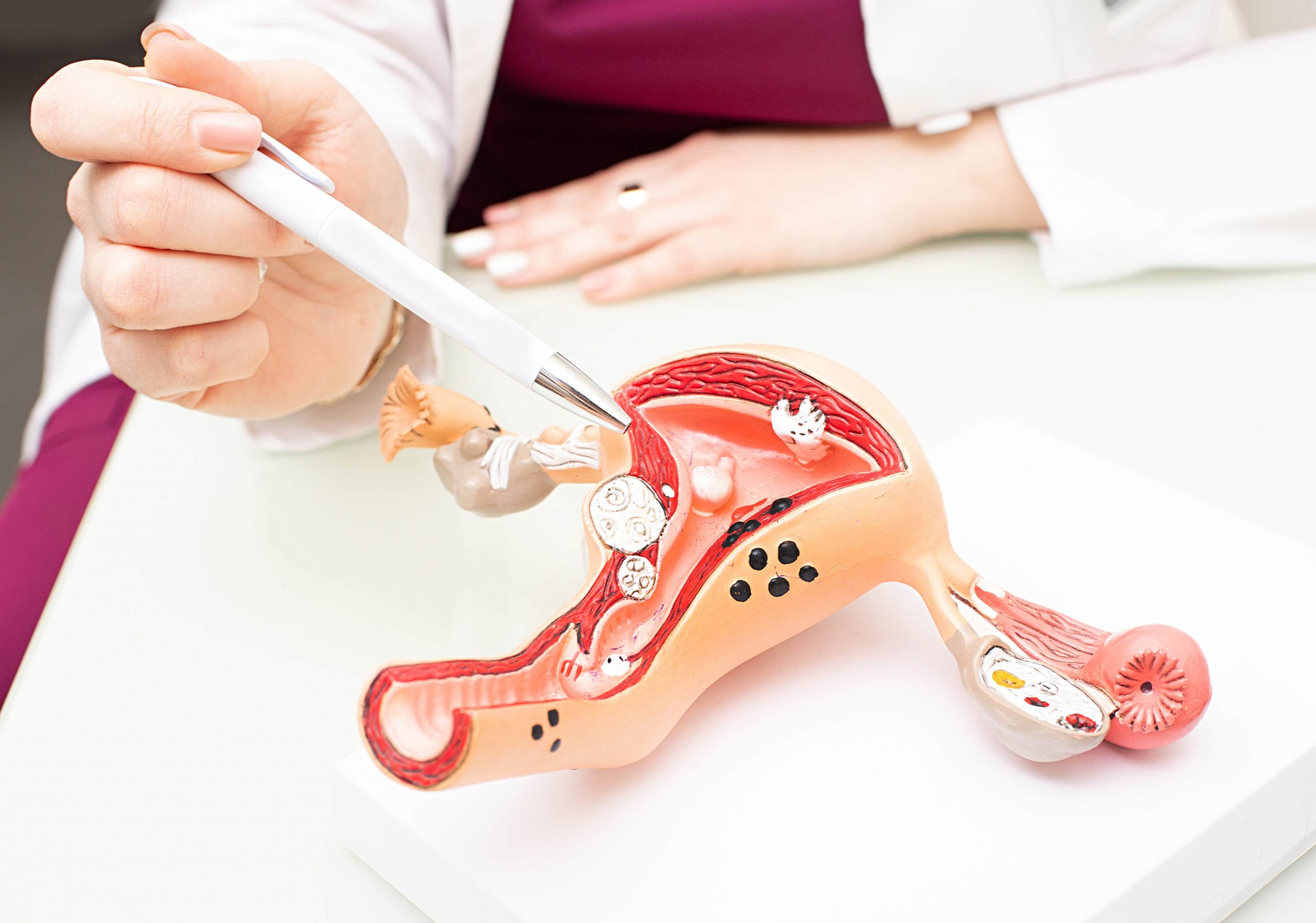
Physical Exam and Medical History
If you develop any signs of endometrial cancer (See Signs and Symptoms of Endometrial Cancer), it is important to consult with your doctor. Your provider will want to know more about your risk factors, symptoms and medical history. You will also receive a pelvic exam and a general physical.
Consulting With a Specialist
If there is a possibility that you have developed endometrial cancer, it is important to have an examination performed by a gynecologist, a doctor who specializes in the treatment and diagnosis of female reproductive diseases. These doctors are capable of treating cases of endometrial cancer, whether these are early or advanced. You may need legal help if there is a failure to diagnose endometrial cancer at an early stage.
Ultrasound
One of the first tests performed is a look at the fallopian tubes, ovaries and uterus in women who may have gynecologic issues. Ultrasound can take pictures of the body through sound waves. A small probe or transducer is used to emit sound waves, and it can pick up the echoes caused by these waves as they bounce off of the organs. Computers can translate the echoes into pictures.
With a pelvic ultrasound, the probe or transducer is placed on the lower abdomen. The bladder will need to be full for the ultrasound to create clear pictures of the ovaries, uterus, and fallopian tubes. For this reason, it is important to drink plenty of water before an ultrasound exam is performed.
A TVUS or transvaginal ultrasound is typically used to look at the uterus. The TVUS probe is typically put directly into the vagina for the for this test. It will be possible to determine whether there is a tumor in the uterus by analyzing the images produced in the TVUS or if the endometrium has thickened, which is a common symptom of endometrial cancer. It can also be used to determine whether the cancer has grown into the myometrium or the muscle layer of the uterus.
Saline (salt water) can be put into the uterus via a small tube just before the ultrasound so that the uterine lining can be more clearly seen by the doctor. This is also known as a hystero- sonogram or a saline infusion sonogram. Sonography can also be used by doctors to identify the areas that should be biopsied, should other procedures fail to detect tumors.
Sampling Endometrial Tissue
To learn whether endometrial cancer or endometrial hyperplasia exists, doctors have to remove a small amount of tissue and look at this under a microscope. Dilation and curettage (D&C) and endometrial biopsy are two ways in which endometrial tissue can be collected. A gynecologist or other specialist can handle these procedures that are detailed below.
Endometrial Biopsy
An endometrial biopsy is a test most commonly performed for identifying endometrial cancer, and it tends to be quite accurate when used in postmenopausal women. During an endometrial biopsy, a small, flexible tube is passed through the cervix and into the bladder. Suction is used to extract a small quantity of endometrium through the tube. The suctioning is usually complete in under a minute. The discomfort caused by this process can be likened to menstrual cramping. It can be alleviated by taking ibuprofen or another non-steroidal anti-inflammatory just before the biopsy is performed. Local anesthetics for numbing the targeted area sometimes injected into the cervix to limit the resulting discomfort.
Hysteroscopy
During a hysteroscopy, a tiny telescope measuring approximately 1/6 of an inch in diameter is passed through the cervix into the uterus. To see clearly into the uterus, doctors will often place saline (salt water) inside of the uterus. This allows doctors to identify and biopsy any abnormal growths such as polyps or cancer. This is often done while the patient is awake. However, a numbing medicine (local anesthesia) will be used.
Dilation and Curettage (D&C)
If an insufficient tissue is obtained through an endometrial biopsy or if the biopsy suggests that cancer is present, but the results are not certain, it will be necessary to have a D&C performed. This is an outpatient procedure in which the cervix is dilated so that a special tool can be used to scrape off uterine tissue. This can be performed with a hysteroscopy or without one.
It takes about one hour to complete a dilation and curettage. This could require general anesthesia (where the patient is put to sleep) or occur under conscious sedation (where intravenous medication is used to make the patient drowsy). Both are performed either in conjunction with an epidural or local anesthesia in the cervix. D&C is commonly performed as an outpatient surgery. This procedure usually causes only a nominal amount of discomfort.
Endometrial Tissue Testing
Endometrial tissues that have been removed via D&C or biopsy can be checked under the microscope for signs of cancer. If cancer is identified, the lab will report the type and state of endometrial cancer (such as whether it is clear cell or endometrioid) along with the grade of cancer.
Endometrial cancer can receive a grade of one to three, based upon how comparable it is to normal endometrium. (This information can be found in What Is Endometrial Cancer). Women who have lower grade cancer are not likely to have recurrences or advanced disease.
If hereditary non-polyposis colon cancer (HNPCC) is suspected by the doctor as being the cause of endometrial cancer, tissue from the tumor can be tested for protein or DNA changes that can occur when the genes responsible for HNPCC are at fault. If these DNA or protein changes are identified, the doctor will recommend speaking with a genetic counselor to discuss genetic testing. Testing for MSI or low mismatch protein levels is often required in women who receive diagnosis of endometrial cancer at relatively young age or who have family histories of colon or endometrial cancer.
Tests To Determine Cancer Spread
When the cancer is believed to be advanced by the doctor, is often necessary to have additional tests performed to determine the cancer spread.
CT or Computed Tomography
The CT scan is an x-ray procedure that is used to create in-depth, cross-sectional images of the patient’s body. During a CT scan, you will lie down on a table while having pictures taken by an x-ray. Rather than taking only a single picture, much like the typical x-ray, the CT scanner can take multiple pictures while the camera rotates around. These pictures are then combined in a computer to produce an image of a slice of the patient’s body. Pictures will be taken by this machine of many slices of the body part that is being researched.
It is necessary to drink between one and two pints of a liquid called an oral contrast before these pictures are taken. This outlines the intestine so that some areas are not mistakenly identified as tumors. Various forms of contrast dye (IV contrast) will be given through an intravenous line. This better outlines various structures throughout the body.
You may experience some flushing as the result of this injection, which typically lasts anywhere from several hours to a few days. Some people are allergic to this dye and may develop hives. In rare cases, serious reactions can occur such as difficulty breathing or low p
MRI or Magnetic Resonance Imaging
Rather than using X-rays, MRI scans use strong magnets and radio waves. Radio wave energy is absorbed and released in a pattern that is determined by specific diseases and tissue types. These patterns can be translated by computers into detailed images of the body part. Much like a CT scanner, it produces cross-sectional slices of the patient’s body, and it can also produce slices that are parallel to the body’s length.
MRI scans are very beneficial for viewing the spinal cord and brain. There are some doctors who believe that an MRI is also effective for learning whether endometrial cancer has grown into the uterus and how far. MRI scans can also be used to identify enlarged lymph nodes with an innovative technique that uses small iron oxide particles. These are injected in a vein and can be spotted by the MRI once they have settled into the lymph nodes.
In many instances a contrast material is placed in the vein, much like it is with a CT scan. The contrast that is used in MRIs is not the same used for CT scans. Therefore, if a patient is allergic to one contrast, this does not mean that she is automatically allergic to the other. MRI scans tend to cause more discomfort than do CT scans.
They take a bit longer and can last up to an hour. It is also necessary for patients to be placed inside of a tube, which can be disturbing for those who are afraid of small, confined spaces. There may be access to open MRI machines. However, these do not produce images of the highest quality. The MRI machine additionally makes a buzzing or thumping noise that some patients find disturbing.
It is possible to block these sounds out by wearing headphones throughout the procedure.
PET or Positron Emission Tomography
Radioactive glucose is given in this test to search for and identify cancer cells. Given that cancers use sugar at a much higher rate than normal healthy tissues. Radioactivity will often concentrate within the cancer cells.
The radioactivity deposits can be spotted by a scanner. This test is most effective for identifying minute collections of cancerous cells. Special scanners fuse CT and PET scans to accurately identify the areas in which the cancer has spread. PET scans are not commonly a part of the make-up for the endometrial scanner that is still in its formative stages. It is often used for more advanced cancers.
Proctoscopy and Cystoscopy
If women develop symptoms that suggest that the cancer has traveled to the rectum or bladders, a lighted tube can be used to examine the insides of these organs. A tube can be placed through the urethra and into the bladder for cystoscopy. The tube is placed inside of the rectum for proctoscopy. Through these exams, doctors can search for the signs of potential cancer. It is additionally possible to remove small samples of tissue during these procedures to put these through microscopic (pathologic) testing. A local anesthetic can be used for these procedures. However, most people receive general anesthesia. You can learn more about what to expect before, during and after these procedures by talking with your doctor. While frequently used as part of the diagnostic process in the past, these procedures are not commonly used as part of current work-ups for endometrial cancer.
Complete Blood Count and Blood Testing
The CBC or complete blood count is a form of blood testing that is used to quantify the different cells in the blood, such as platelets, white blood cells, and red blood cells. Endometrial cancer can result in anemia or low red blood cell counts due to the bleeding that this cancer causes.
CA 125 Blood Test
CA 125 is a substance that many ovarian and endometrial cancers release into the blood stream. If women have endometrial cancer, a significantly elevated blood CA 125 level often means that the cancer has traveled outside of the uterus. Prior to surgery and most other forms of cancer treatment, many doctors will review CA 12 blood levels. If these are very high, they can be checked again in the future to gauge the efficiency of the treatment method. For instance, levels might fall after a surgical procedure if the cancer has been removed successfully.
CA 125 levels are not necessary for an endometrial cancer diagnosis. Thus, this test is not ordered for every patient.